Shock
About Shock
Shock is a life-threatening condition that occurs when the circulatory system (which distributes oxygen to the body tissues and removes waste products) fails and, as a result, vital organs such as the heart and brain are deprived of oxygen. It requires immediate treatment to prevent permanent organ damage or death.
Shock can be made worse by fear and pain. Whenever there is a risk of shock developing, reassuring the casualty and making them comfortable may be sufficient to prevent them from deteriorating.
The most common cause of shock is severe blood loss. Loss of other body fluids from conditions such as diarrhoea, vomiting or severe burns can also result in shock.
Shock may also occur when the heart is unable to pump blood. This may be due to severe heart disease, heart attack, or acute heart failure. Other causes of shock include overwhelming infection, lack of certain hormones, low blood sugar (hypoglycaemia), hypothermia, severe allergic reaction (anaphylactic shock), drug overdose, and spinal cord injury.
Effects of Blood or Fluid Loss
| Approximate volume lost | Effects on the body |
| 0.5 litre (about 1 pint) | Little or no effect; this is the quantity normally taken in a blood donor session. |
| Up to 2 litres (3.5 pints) | Hormones such as adrenaline are released, quickening the pulse and inducing sweating; Small blood vessels in non-vital areas, such as the skin, shut down to divert blood and oxygen to the vital organs; Shock becomes evident. |
| 2 litres (3.5 pints) or more (over a third of the normal volume in the average adult) | As blood or fluid loss approaches this level, the pulse at the wrist may become undetectable; Casualty will usually lose consciousness; Breathing may cease and the heart may stop. |
Look for:
Early stage:
- A rapid pulse
- Pale, cold, clammy skin
- Sweating
- Chattering teeth
Developing stage:
- Grey-blue skin (cyanosis), especially inside lips. A fingernail or earlobe, if pressed, will not regain its colour immediately.
- Weakness and dizzyness
- Nausea, possibly vomiting
- Thirst
- Rapid, shallow breathing
- Weak pulse. When the pulse at the wrist disappears, about half of the blood volume will have been lost.
Final stage:
- Restlessness or agressiveness
- Yawning, gasping for air
- Unconciousness
Finally, the heart will stop.
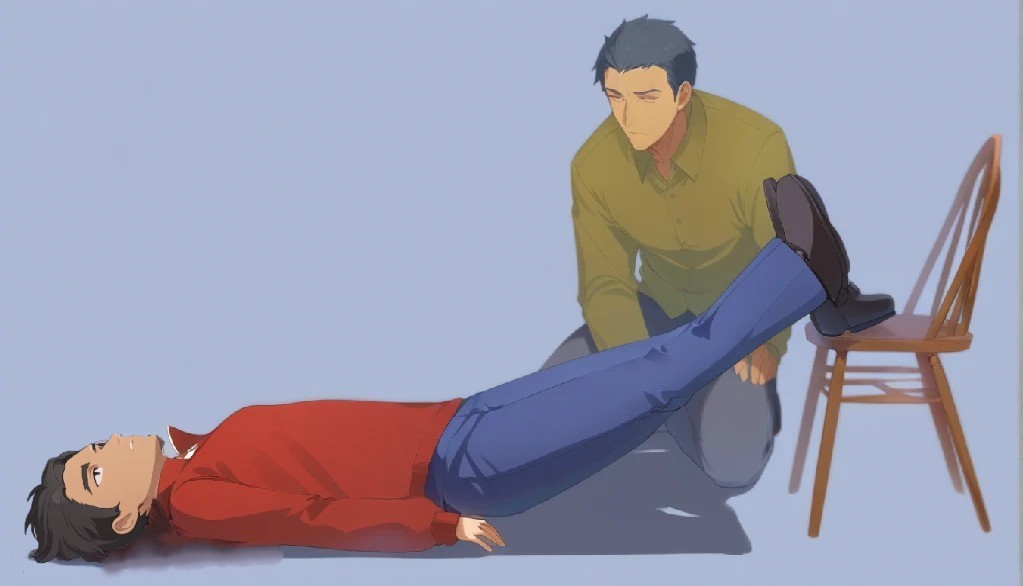
STEP 1: HELP CASUALTY TO LIE DOWN
- Lay the casualty down and use a blanket to help insulate them from the ground.
- Raise and support their legs as high as possible.
- Keeping the head low and the legs high directs blood flow to the vital organs (heart and brain) and may prevent the casualty losing consciousness.
- Treat any cause of shock, such as bleeding.
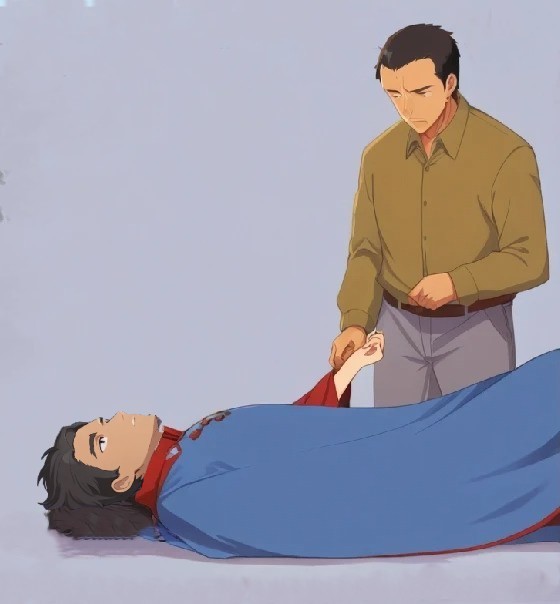
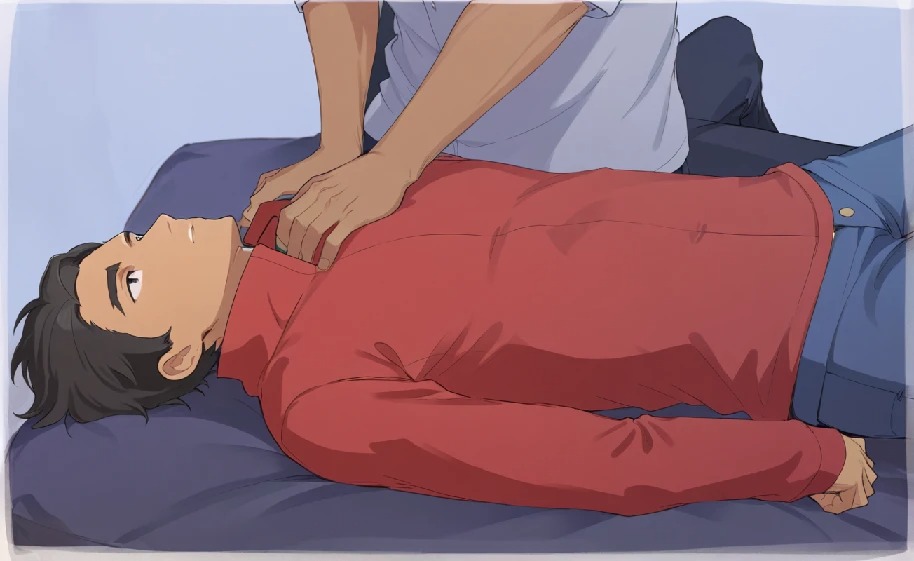
STEP 2: LOOSEN TIGHT CLOTHING
- Undo anything that constricts their neck, chest and waist to reduce constriction of blood flow in these areas.
- Cover them with a blanket to keep them warm.
- Do not allow the casualty to eat, drink, smoke or move unnecessarily – if they complain of thirst, moisten their lips with a little water.
STEP 3: CALL FOR AN AMBULANCE
- Do not leave the casualty unattended, except to call an ambulance.
- If possible, send a helper to call for an ambulance.
- The caller should give the controller details about the cause of shock, if known.

STEP 4: MONITOR BREATHING, PULSE, AND RESPONSE
- Monitor and record vital signs – level of response, pulse, and breathing.
- If the casualty becomes unconscious, open the airway and check breathing. Be prepared to give chest compressions and rescue breaths.